Getting an epidural during labor is a very common form of pain mangement in the US. Today I want to talk to you about what it will do for you, how it is placed and what to expect throughout the process.

Remember, the epidural is just ONE of the forms of pain management — I think it’s important to know about ALL of them — so grab my pain management options tip sheet here:
Epidurals During Pregnancy
There are a lot of reasons that people get epidurals, but one of most common is to mitigate the pain of labor.
Epidurals are also given for back, limb pain. I actually got it for pelvic pain after my last baby.
They are also frequently used in surgery (although more often a spinal is given for a cesarean section anesthesia).
Benefits of an epidural during labor
The main benefit is pain relief. You should expect 80% of labor pain to be taken away from the epidural.
The epidural, when place correctly COULD Take away all the pain you have. However…. only taking away 80% allows you to:
- Pain feedback may allow labor to progress (your body knows something is happening vs having all the receptors numb)
- Help us move you (it is really hard to adequately move dead weight if you were 100% numb)
- Help you to know if baby is lower in your pelvis
- Push more effectively
That does mean you should expect some discomfort even after the epidural is placed. Which is why I recommend some natural pain management techniques even if you plan on an epidural.
By taking away the pain. The mother is able to rest during labor, and baby isn’t subject to a lot of stress hormones if mom were to get out of control.
Risks of an epidural during labor
The biggest risk is a spinal headache. That means the doctor goes a bit too far with the need, and allows some spinal fluid to leak out.
There are a lot of tell-tale signs of a spinal headache. The biggest one is no pain when you are flat, but when you lift your head, the headache returns.
Your anesthesiologist can do a “blood patch” that can help your spinal headache feel better.
Of course, your doctor will review an entire informed consent including irritation or infection at the placement site up through death.
And yes, a proper informed consent does need to include death. As it would every time you got in your car or turned on your oven.
While the pain is a big worry for a lot of people, most people are traumatized by not being able to communicate with their team like they had hoped to (and feel forced into choices). I talk about that in here << THAT is what prevents birth trauma!
What do you need to get an epidural?
Before an epidural you will need:
- Labwork we especially need to know if your platelets are enough (so you don’t bleed)
- An IV (we give you about a full bag of extra fluid before placement to prevent your blood pressure going down)
- A doctor’s order — some providers don’t allow patients to get an epidural until their cervix is at a certain amount.
If you have questions about when your doctor would order an epidural please consider talking to them at your appointment.
Also, if you have any questions about any back issues, or scoliosis, you can talk with your OB/provider at your prenatal appointments. If the OB is concerned they can sometimes order a consult with you and an anesthesiologist before delivery.
Epidural Placement Procedure
The epidural placement is an area of great concern for many pregnant women as it sounds much worse than it is.
For your part (as this isn’t a post on training anesthesiologists) you will likely sit up. Some anesthesiologists have you lay down and place it with you on your site, but most have you sit up.
They will feel your spine and your hips possibly drawing some marks on your back for ease of placement.
Then, they will prep the area with soap (will feel very cold) and a drape. Once it is cleaned and draped, this area is sterile and you want to be very careful not to touch back there.
Between the anesthesiologist (an epidural can also be placed by a nurse anesthetist) and your nurse they will help you to position during the placement.
The best position to be in is with a rounded back with your shoulders down. I help my patients picture it like a shrimp, or a mad cat — you’re really trying to push the middle area of your back out at the doctor.
Easier said than done with a baby in front of you.
Once they feel your position is appropriate they will numb you a bit with lidocaine. This is the most painful part, and most people compare it to several bee stings. This will numb that area for the placement, to make the procedure less painful overall.
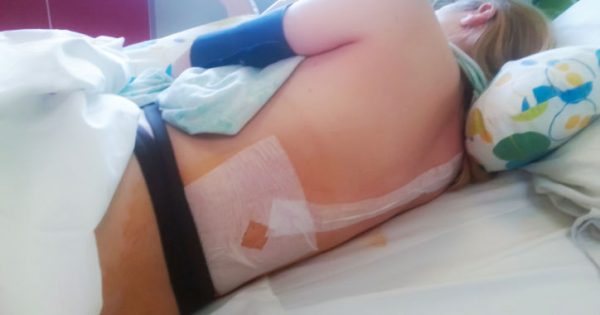
After the epidural is placed (takes anywhere from 5-30 minutes most often once drape is applied) the needle is removed and a flexible catheter is placed in your back.
Pro Tip: The needle is removed from your back, and just a flexible tube is left — so you can (and should) still move in the bed).
After that they will use several layers of take and dressing to keep it secure in your back.
It is important to try not to drag your back across the bed after it is placed. Some MD’s compare it to treating your back like it has a sunburn (you’d lift up and move it vs dragging it across the sheet).
How much does it hurt to get the epidural?
I think the epidural hurts very similar to the IV placement. You will need an IV before getting an epidural.
While we’re here — have you thought about pain management on your birth plan — let me help you out here:
Expectations of the patient during epidural placement
Our biggest expectation is that you will remain still while the needle is in your back.
If you are not still there are obviously concerns about the needle going to far, which could be extremely problematic.
I have had patients who were unable to maintain the position and they were unable to get an epidural.
This sounds miserable, but keep in mind that it usually only happens during 2-3 contractions, and then they will start to feel shorter and less intense. Most women don’t have too much issue remaining still realizing that they will have a benefit in not too long.
Honestly, most patients do pretty well with it.
Partner during epidural placement
Most often only one support person is allowed in the room (although, I have heard that sometimes no one else is allowed in the room)
That person most often has to sit during the placement either at the other end of the room or in front of you.
I often place dads in front of mom so she can put her feet on his knees during the placement. It makes it easier for them to curl their back up.
It is VERY important that the procedure be 100% sterile, so support partners would not be able to be back near the anesthesiologist. They should be there to be a support to you, and tell you how great they are doing.
The reason we have them seated is that some partners feel a bit woozy, and the nurse can’t as easily watch dad during placement because she will be helping anesthesia and you. So, to prevent any falls/fainting we ask them to sit in chairs.
Some facilities may require your partner to leave, so you can ask them what their usual protocol is.
I actually go through the whole process of how they put in the epidural (and I do it with some household items and Raggedy Anne) in here.
Expectations of the epidural after placement
What will it feel like after the epidural is in?
How long does it take to feel “numb”?
Most often within 20 minutes the epidural starts to “set up”. Often, it does set-up unevenly and it takes a bit of time for both sides of the patient’s body to feel similar.
Epidural trouble-shooting
The epidural does run with gravity, so it is important that you don’t stay on one side for TOO long after placement. Most nurses turn their patients every hour or so. Sometimes turning you to a side that hurts more can help.
Most epidurals are run on a PCA pump anymore. This means that the patient has control of how much medication they are getting. Our patients have a “button” they can push to get more medicine if they are hurting more than they would prefer. This only allows extra medicine to be given ever x number of minutes, so you don’t end-up getting too much.
However, if you are finding that you are pushing the button frequently, we can also have anesthesia increase the rate of epidural medication.
Sometimes the epidural catheter can be pulled out a tiny bit and that can help the infusion (sometimes there could be a kink inside your back).
Also, sometimes the epidural will need to be replaced.
Most of these options need to be considered by anesthesia (besides the PCA button) — so if you feel like the epidural is not working ask to directly speak with the anesethesiologist.
Often, they want the nurse to troubleshoot, but there are limited things the nurse can do — and bare in mind that you are paying anesthesia a LOT of money (sometimes even more than your OB) to place and run that epidural. So, they should be actively managing it and you should be getting that 80% of pain relief.
How do you pee after the epidural?
A foley catheter is place after the epidural because you would not be able to lift to use a bed pan (you also might not be able to release your urine) or walk to the bathroom.
A foley catheter is a tube that goes up into your bladder and drains the urine for you. It is most often put in after you are numb and taken out before you start to push.
You need to empty your bladder effectively to clear a path for the baby (as the bladder can get in the way of baby’s head descending).
BTW, if you’re looking for more info on technical stuff like this and the foley catheter — I’d 100% recommend joining this course.
Epidural After Labor
After you have the baby, and most often once any stitches are placed they will turn off the epidural.
Once you are in a spot where you can sit up your nurse will take the epidural out. She will also check the tip to make sure that it comes out intact (as that could obviously be an issue).
You may have some soreness in the area as you have had the skin pierced. You’ll also have similar pain around your epidural site.
You may also have some bruising. I also feel it when water hits in the shower (like a bruise).
Back pain after labor with epidural
Some women say they have back pain due to an epidural.
This is possible, although unlikely as the doctors are very skilled that place it.
Studies show that there is not increased back pain (after a couple of months when the bruising is gone) from those who had an epidural vs those who did not.
Motherhood with a newborn is FULL of bad positioning. Carrying the carseat. Leaning over to nurse. Leaning over to put the baby in the crib or changing diapers. Not to mention the weird positions we find ourselves asleep in.
It’s just a lot of poor mechanics. So be mindful of your back. It is more like you you vs the epidural.
If you made it this far you really want to know about what’s going to go on at the hospital. The Online Prenatal Class for Couples really is the easy way to get prepared for birth. It has a full chapter on medication pain management and then another bonus video on natural pain management options. You won’t want to miss either one!
Have you checked a birth class off your to do list✅? I have a few I recommend:
❤️ Best class for couples {per BabyList}
👩💻 Best class available on demand
⚡ Best class JUST for pain management
👶 Best Postpartum-Only Prep
❤️🧡💛💚💙💜 My favorite class is here.
Now is the time to get started!
Want to do a vibe check before diving into the whole thing with me? — check out my free labor pro tips. It’s your first step toward getting in the driver’s seat of your birth.













 What Happens if Your Induction Doesn’t Work?
What Happens if Your Induction Doesn’t Work?

[…] sure to check out my whole post on epidurals in labor — it’s super helpful to learn more about […]